
Influenza Pandemic Planning
This site provides links to local (Hunter New England Health), State, National and International plans, policies and documents to improve preparedness for pandemic influenza.
Being prepared will help reduce the effects of a pandemic.
- Information for general practitioners and healthcare workers
Includes fact sheets, general information, treatment, useful web links - Information for businesses
Link to a range of tools to help your business prepare for an influenza pandemic or other health emergency - Be prepared
Link to information about preparing in case of an emergency or a disaster
Pandemic preparations
Adverse Event Following Immunisation
An adverse event following immunisation (AEFI) is an unwanted medical reaction after administration of a vaccine, which may or may not be related to the vaccine. Adverse events may be at the site of injection, a general illness or a general allergic reaction.
AEFIs are notifiable conditions under the NSW Public Health Act (2010). Notification is required by vaccine providers, doctors and hospitals to the Public Health Units. The general public can self-report directly to the TGA.
The Australian Immunisation Handbook (online edition) provides information about the frequency, types and management of AEFIs. Expected reactions following vaccinations do not need to be reported to the PHU.
Some AEFIs of special interest include:
- Unusual/ unexpected clinical event following immunisation with critical care admission or major impairment
- AEFIs in children that have been hospitalised with a suspected vaccine-related complication within 6 weeks of vaccination
- Anaphylaxis
- TTS/VIPIT cases
- Other disorders of clotting and haemostasis
- Myocarditis/pericarditis
- Guillain-Barré syndrome (GBS)
- Bell's palsy
- Other new onset neurological disorders
- Hearing loss/Tinnitus
- Extensive Limb Swelling (ELS)
- Hypotonic-Hyporesponsive episode (HHE) (in children <1 year age)
In NSW the national AEFI reporting form is to be returned to your local Public Health Unit (PHU) for investigation and recommendations on future vaccinations. Ensure you include all relevant information such as, specialist reports, photos and pathology. To make a notification please complete the National Reporting Form and email to the HNE Population Health Unit at HNELHD-PopHealthAEFI@health.nsw.gov.au
Patients who would like to self-report a non-serious AEFI are encouraged to report direct to the TGA.
Resources:
HNE AEFI Email address: HNELHD-PopHealthAEFI@health.nsw.gov.au
HNE PHU contact number: 1300 066 055
TGA National Reporting Form
Self-Report FormTherapeutic Goods AdministrationAustralian Adverse Drug Reaction Reporting System (tga.gov.au)
Australian Immunisation Handbook – under each disease chapter is a list of expected reactions The Australian Immunisation Handbook (health.gov.au)
Catch-up Vaccination
- Catch-up Calculator | The Australian Immunisation Handbook (health.gov.au)
- Additional vaccines provided free in NSW Additional Commonwealth and NSW-funded free vaccines - Immunisation programs
Catch-up vaccines for refugees and humanitarian entrants aged 20 years and over (ongoing)
The Australian Government has extended the provision of free catch-up vaccines for refugees and humanitarian entrants aged 20 years or over through the National Immunisation Program. Detailed information is available in the Vaccination Provider Factsheet (refugee catch up) Free catch-up vaccines for refugees and humanitarian entrants aged 20 years and over fact sheet | Australian Government Department of Health.
Catch-up schedules for people with no previous vaccinations
Generic catch-up templates for individuals with nil evidence of previous vaccinations and nil contraindications. Check AIR to ensure no previous vaccines have been administered.
(the following are exclusive pdfs that we have created, they aren’t available as links)
Cold Chain Breach
Save the completed form with your surgery name and attach the completed form to your return email.
Download the Cold Chain Breach Reporting Form to report a cold chain breach. (disregard temperatures < 12 degrees for < 15 mins)
ACTIONS
- Place sign on vaccine fridge stating DO NOT USE and DO NOT DISCARD
- Download data logger and save on your computer
- You will need to save the form on your computer first, then complete the required information. Save the completed form with your surgery name.
- You will need to attach it to your return email. Do not return printed or faxed copies of this reporting form.
- Ensure a detailed description of the CCB is provided in section 2 to assist with the assessment of the breach.
- In Section 4 you will need to report vaccines that have had a previous CCB. All vaccines exposed to a second breach ( that is vaccines with cold chain breach stickers already applied) need to be reported in brackets. For example, today's breach has 7 doses of Priorix and 5 of those have a sticker from an earlier cold chain breach.

- THEN return the following completed forms to Hunter New England PHU by email to
hnelhd-phimmunisation@health.nsw.gov.au
- Completed Cold Chain Breach Reporting Form
- Data loggings for the duration of the cold chain breach. Preferably attached the “live” data logger file. That is the colour file that you save to your computer
- Vaccine refrigerator twice daily min/max temperature chart
- And any other attachments as per the Cold Chain Breach reporting form “Attachments Required”
Once all documents are returned the PHU will:
- complete section 4 and the PHU Use Only section advising your service which vaccines are to be retained and labelled, which vaccines are to be discarded and any other requirements.
- Submit your wastage report to the NSW Health State Vaccine Centre.
Please Note:
- Do not attempt to reorder vaccines until this cold chain breach is finalised.
- For advice on private vaccines- you will need to contact the vaccine manufacturer.
Thank you for your cooperation.
Maintaining Authority to Immunise
It is your responsibility to keep your practice current. For your General Nursing Registration you are required to have at least 20 hours of documented learning. Some of these hours can include immunisation education.
To maintain your authority to immunise, ‘the registered nurse/midwife annually reviews best practice policy for immunisation. This may be, but is not limited to, attendance at seminars on current practices. An annual statement of proficiency in cardiopulmonary resuscitation must also be obtained’ (from Authority for Registered Nurses)
Activities that would assist in fulfilling these requirements include:
- Reading To the Point Newsletter (see tab below)
- Completing the cold chain online module ’Vaccine Storage and Cold Chain Management’ Cold Chain Management (Updated)V5WEBHTMLFlash (seertechsolutions.com.au)
- Education Updates - HNELHD will hold education sessions throughout the year, these will be advertised in our To The Point Newsletters and on our website under Immunisation Education. Past webinars available here Immunisation Education under Educational Updates. These are not mandatory.
- Journal articles, media releases, faxes, online resources etc
Further details available from the Nursing and Midwifery Board (Ahpra) - Continuing professional development Guidelines Nursing and Midwifery Board of Australia - Guidelines: Continuing professional development (nursingmidwiferyboard.gov.au) Document your Learning on provided record or available apps.
Overseas Vaccination
COVID- 19 vaccines are approved for use in Australia by the Therapeutic Goods Administration (TGA). The TGA have approved or recognised some COVID-19 vaccines given overseas, and are continually reviewing other vaccines that may be recognised for the purposes of inbound travel to Australia in the future.
If a patient has been vaccinated overseas and cannot get an International COVID-19 Vaccination Certificate (ICVC) yet, when travelling to Australia they can use their foreign vaccination certificate.
Guidance on foreign vaccination certificates
Guidance on foreign vaccination certificates | Australian Passport Office (passports.gov.au)
If a patient has received an approved vaccine while overseas, they can have it recorded on the Australian Immunisation Register (AIR) when they return to Australia. It will then appear on their immunisation history statement. Services Australia can assist customers with adding approved overseas vaccinations to the AIR.
Current approved and recognised vaccines for COVID-19 | NSW Government
There is no requirement for providers to add an overseas history for a person if they are still residing outside of Australia.
As per the Australian Government Department of Health, it is mandatory to report all vaccines to the Australian Immunisation Register (AIR). The Australian Immunisation Register Rule 2015 outlines the reporting requirements, which includes reporting to the AIR within 24 hours and no more than 10 working days after vaccination. This includes the presentation of a vaccination history administered outside Australia. The Australian Immunisation Register Rule 2015 states that if a recognised vaccination provider is given information about a relevant vaccination that was administered outside Australia, the provider must report within the period prescribed by the rules.
Individuals aged < 20 yrs may have some Centrelink payments linked to vaccinations received overseas which have not yet been recorded on the Australian Immunisation Register (AIR).
All vaccines given overseas should be added to the AIR. If any vaccinations are listed as overdue (missing) on the AIR, a catch-up schedule will need to be developed.
STEPS:
- Ask parents/carers to provide evidence of vaccines given overseas. Ensure all records are translated into English and dates are available. (You may need to Google brand names to establish antigen content.)
Translating overseas immunisation encounters
The Australian Government offers a free translating service that can be used by anyone who holds a permanent visa. GPs and medical specialists can also access the Australian Government Department of Home Affairs Free Interpreting Service Translating and Interpreting Service (TIS National) when providing Medicare-rebateable services. - Add all records onto the AIR Vaccination schedules from other countries (WHO)
http://apps.who.int/immunization_monitoring/globalsummary/schedules
HOW TO ADD RECORDS TO THE AIR
Use the Identify Individual option in the left-hand menu to search for an individual.
If the individual is enrolled in Medicare, the quickest way to locate their AIR record is using their:
- Medicare number and
- Individual Reference Number (IRN)
If they aren’t enrolled in Medicare, look up the individual by entering:
- surname
- first name and
- date of birth
If the AIR finds a unique match, the Individual details page will display the individual's immunisation details.
If you have just created a new person on the AIR just record ONE encounter initially (not a birth dose, so eg, the 6 weeks vaccines).
Either (depending on urgency):
- wait 20 min, phone the AIR on 1800 653 809 and request the person’s record be made ‘live’. This means you can then go back and search for the person on AIR then add remaining vaccine encounters
OR
- wait 48 hours and search on AIR for the person, then add remaining vaccine encounters
Once you identify the individual or create a new record, you can record an encounter or update a previous encounter.
Put in one encounter, wait 48 hours and look for the child again, when there add all other encounters
If the AIR can't find a unique match, you should:
- check you’ve entered the details correctly
- add a postcode
- select Search again
If the AIR still can't find a match, you can create a new record.
Select the Record Encounter button located on the bottom right-hand corner.
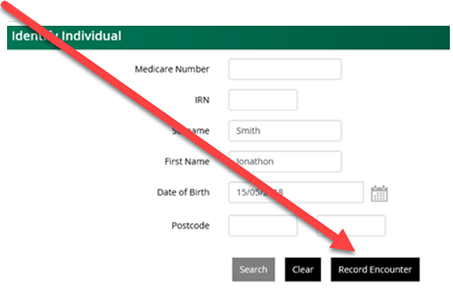
Once you identify the individual or create a new record, you can record an encounter or update a previous encounter
Record encounter
- Who performed this immunisation encounter? Select This encounter was performed overseas
- Schedule - select Other from the dropdown menu.
- Date of Service -Enter the date the individual received the vaccine.
- This Date of Service applies for all episodes - can uncheck this box if you need to record a separate date
Tip: Fields with a red asterisk are mandatory - Vaccine or brand - If you don’t know the vaccine brand or it’s not listed, choose the ‘generic’ vaccine.
Tip: You can enter up to 3 NIP schedule vaccines and 5 non-NIP vaccines for each encounter. - Batch Number -This field is optional, however, we recommend you enter the Batch Number
- Dose - You must enter a Dose number for all episodes not part of a schedule.
When you’ve entered all the required details, select the Add button to record the vaccine. You’ll then see the recorded episode details. - Once records have been added to AIR, check to see which vaccines are missing
- Develop a catch-up plan and vaccinate as required.
- Serology may be an indication in some situations - refer to generic catch-up templates.
If catch-up cannot be achieved in one visit and further visits are planned tick the ‘Planned Catch up’ box on the AIR for that child. This allows Centrelink payments to continue for 6 mths.
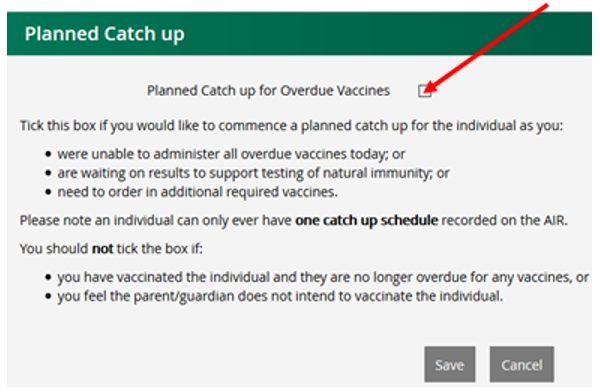
If you require further assistance, please contact the immunisation team.
Rabies or Australian Bat Lyssavirus
Contact the PHU on 61 2 4924 6477 immediately to report potential contact with bats in Australia or mammals overseas.
Information required to initially report contact:
- Name, DOB, contact number
- Details of animal and type of contact
- Immunosuppression
- Weight
- Previous vaccination
Do not send patients to emergency departments. There is no maximum time between exposure and treatment.
Travel Vaccination
The HNE Public Health Unit does not provide a travel vaccination service. Refer patients to specialist travel GP facilities (such as Authorised Yellow Fever Vaccination Providers In NSW)
Useful Travel Links:
Vaccination Records
All vaccines administered in Australia should be available for viewing on the Australian Immunisation Register (AIR). Assistance accessing these records can be found here:
School Vaccination Records
Most school records with the exception of vaccines administered in some Local Health Districts, in the current school year are available on AIR. If you believe a school vaccination has been administered and is not visible on the AIR, complete the Request for school vaccination records be added to the Australian Immunisation Register (AIR) form.
Frequently Asked Questions (FAQ)
My child missed a vaccine in the school program, what happens now?
Students who miss vaccine doses due to absence on the day of the nurses' visit will be offered catch-up vaccination at subsequent school clinics. Where this is not possible, parents will be advised that a free catch-up vaccine is available at their local GP.
I need a vaccination summary to enrol my child in a new school and their school vaccinations are not showing on the AIR.
See above regarding school vaccination records.
Vaccine Ordering and Management
If your facility is unable to order vaccines please contact us on 61 2 4924 6477 (eg. If there is a block on your account)
- Vaccine Ordering NSW Vaccine Centre Online Ordering System - Online Ordering System Login (tollhealthcare.com)
- Order New Cold Chain Breach Labels (order extras)

Vaccine Cold Chain Resources
Other Resources
- Adverse Event Following Immunisation (AEFI) Form Adverse Events Following Immunisation (AEFI) | Immunisation programs (nsw.gov.au)
- ASCIA Guidelines to Acute management of Anaphylaxis ASCIA Guidelines Acute management of anaphylaxis | Australasian Society of Clinical Immunology and Allergy (ASCIA)
- Health Care Worker/Student Vaccination Requirements Occupational Assessment, Screening and Vaccination Against Specified Infectious Diseases (nsw.gov.au)
- Injection Site Poster ImmunisationPosterA3_14+JULY.pdf (squarespace.com)
- Letters from Medicare Regarding Missed Vaccinations Australian Immunisation Register | Update your details on your Medicare card and on the AIR | Services Australia
- Tetanus Advice Card - for Tetanus-Prone Wounds A4_size_tetanus_advice_card.pdf (nsw.gov.au)
- To the Point Newsletters
- Vaxtracker
Request for Vaccine Account Number for New Practice
How to Apply for a NSW Ministry of Health Vaccine Account Number (VAN)
- Complete "Immunisation Facility Details Form.docx" and return the completed form to us by email
- Obtain required resources as listed in "Procedure to apply for Vaccine Account Number (VAN) document"
- Ensure each staff member who will be handling vaccines has watched NSW Immunisation cold chain learning module education- link below
- Review downloaded "Procedure to apply for Vaccine Account Number (VAN) document’ and ensure compliance with each recommendation
- For HNE facilitates: Download a copy of HNELHD Policy Compliance Procedure for the Storage of Vaccines In Hunter New England Facilities
- Provide at least three full days of computerised data logging of the vaccine fridge showing temperature recorded every 5 minutes within 2 – 8 degrees
- Request a visit from PHU immunisation nurse – who will assess suitability for vaccine storage and assistance with delivery of vaccination services
Useful Documents
Useful Websites
Please don’t hesitate to contact us with any questions.
The state of preparedness
HNE Health has emergency management plans and organisational arrangements that provide the foundations for managing services during health emergencies.
Each of the eight local health districts in New South Wales (including HNE Health) employs a Biopreparedness Epidemiologist to further develop plans. HNE Health also conducts research that has been used to guide state and national policy. In addition, a number of committees and working groups are responsible for developing contingency plans appropriate for health emergencies, including pandemics. A central Biopreparedness Unit has been set up at NSW Health in Sydney along with internal and external structures to mitigate against the impact of health disasters.
HNE Health has a comprehensive pandemic plan which can be adapted to suit a range of health emergencies. This is a living document that is regularly exercised to ensure health staff are familiar with their duties and responsibilities. Planning for pandemic response strategy can be adapted to suit other disaster situations.
The Commonwealth government and NSW Health have large stockpiles of medical goods including antibiotics, antiviral drugs, personal protective equipment and other equipment necessary for a health response an emergency.
